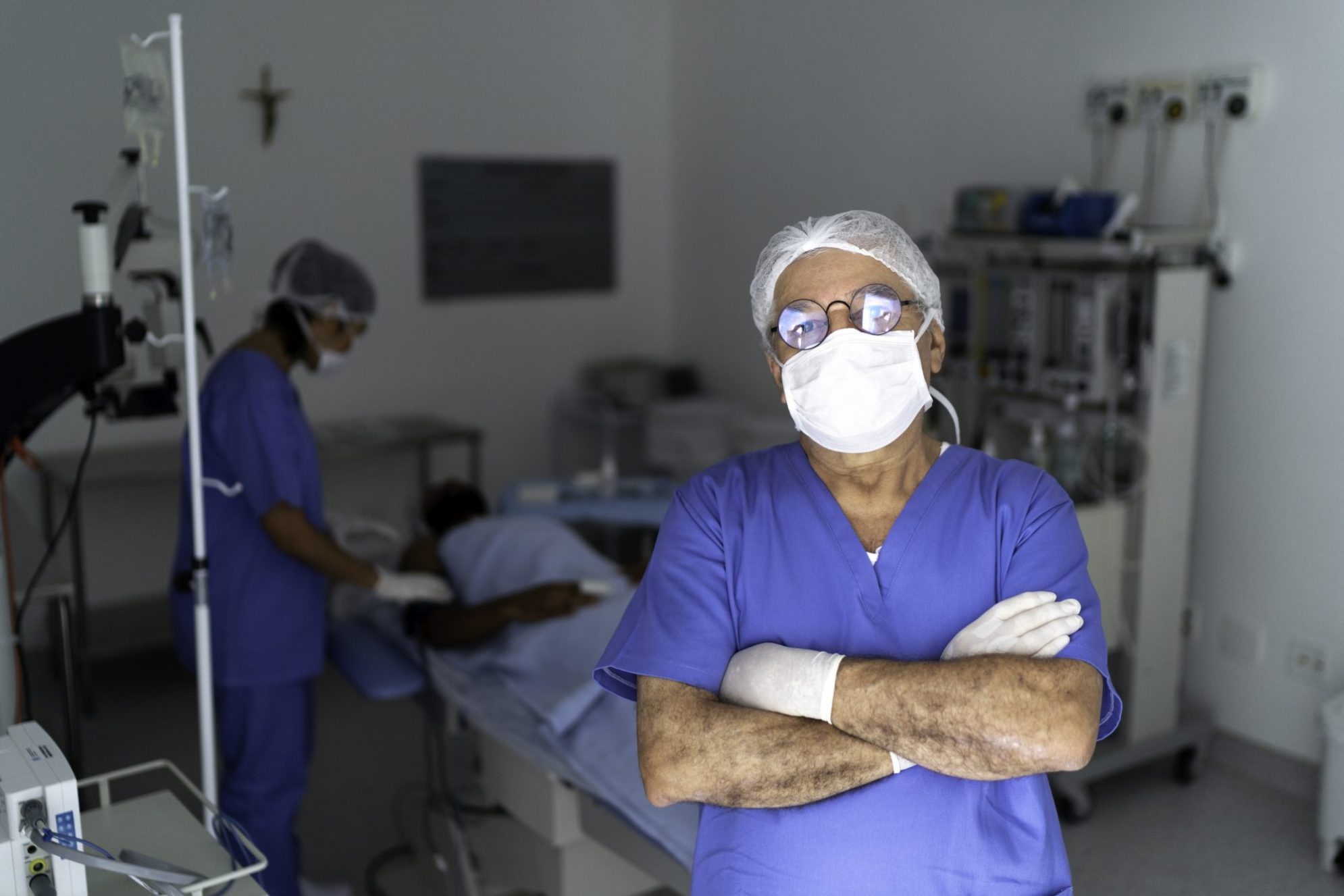
NHS communicators fear crumbling of support
Health communicators are deeply concerned that public support for the NHS may soon start to crumble as the health service wrestles with the daunting task of restoring pre-COVID levels of service, writes John Underwood.
The recent publication of NHS waiting list figures brings home the dramatic degree to which the coronavirus pandemic has changed NHS priorities. The exceptional circumstances of the global pandemic required an unprecedented shift of resources away from routine NHS treatments.
One of the tragic outcomes is that many people will undoubtedly suffer more from the consequences of tackling the pandemic than from the potent effects of the virus itself. It is now likely that cancers, heart disease and mental health problems will go undiagnosed and untreated.
With cases of coronavirus infection now at lower levels – at least for the time being – NHS leaders are working hard to re-establish routine services but with exhausted staff and the need for social distancing in hospitals, as elsewhere, it will be an uphill struggle to see and treat as many patients as before the pandemic, let alone begin the task of tackling the long waiting lists.
This is going to be a major challenge not just for clinicians and managers but for professional NHS communicators too.
Deep concerns
A recent study from the Centre for Health Communication Research at Bucks New University, conducted in conjunction with NHS Providers and NHS Confederation, suggests that health communicators are deeply concerned that public support for the NHS may soon start to crumble as the health service wrestles with the daunting task of restoring pre-COVID levels of service.
The survey of over 160 NHS communication specialists included respondents from across the country and from all types of NHS organisation including hospital trusts, ambulance trusts, mental health trusts, health commissioners and health regulators.
Respondents spoke of the NHS benefitting from a “feeling of reverence” during the early stages of the coronavirus pandemic when the public came out to applaud frontline workers every Thursday evening. But the research indicates a clear concern that the pendulum could swing very swiftly in the opposite direction as the immediate pandemic threat passes.
Comments from NHS communicators were trenchant and to the point. They didn’t pull their punches. They said:
“I think we are going to enter a period soon where the media and public will start turning on the NHS as we are unable to meet expectations of restoring services and seeing people as quickly as they hope.”
“It will… be a difficult transition to get back to ‘normal’ once the national support from the public trails off following huge donations, offers of support, volunteering etc.”
“Perceptions of the NHS will change quickly when the immediate threat passes and stories of 3-year delays of operations, missed cancer diagnoses and waiting lists for mental health services start gaining traction.”
The NHS will change dramatically in the coming months and years and in many respects the pandemic has been a catalyst for the sort of rapid, innovative change that is sorely needed. But the changes ahead may not all be welcomed by members of the public, many of whom are expecting a return to some sort of pre-COVID “normal”.
More services will be delivered digitally, more will be delivered in settings other than hospitals and waiting lists are not going to fall rapidly. A return to anything like pre-COVID normality depends on persuading patients and the public that hospitals are not dangerous places and that many are now largely COVID-free environments.
The challenges ahead for clinicians and managers are significant. They are no less significant for NHS communicators who will need a properly resourced, super-human communication effort if they are to maintain public faith in the NHS.
John Underwood is director of the Centre for Health Communication Research at Bucks New University and Executive Director at Freshwater.
This article first appeared in the HSJ on 24 August 2020.
